NHS Patient Survival Rates Lag Behind Rich Nations Despite Billions

A recent major international analysis has revealed that NHS patients exhibit higher mortality rates compared to those in almost every other wealthy country, despite receiving record levels of funding.
Britain ranks near the bottom of a global league tablefor 'treatable mortality' – deaths considered potentially avoidable with timely and effective healthcare – with only the United States performing worse.
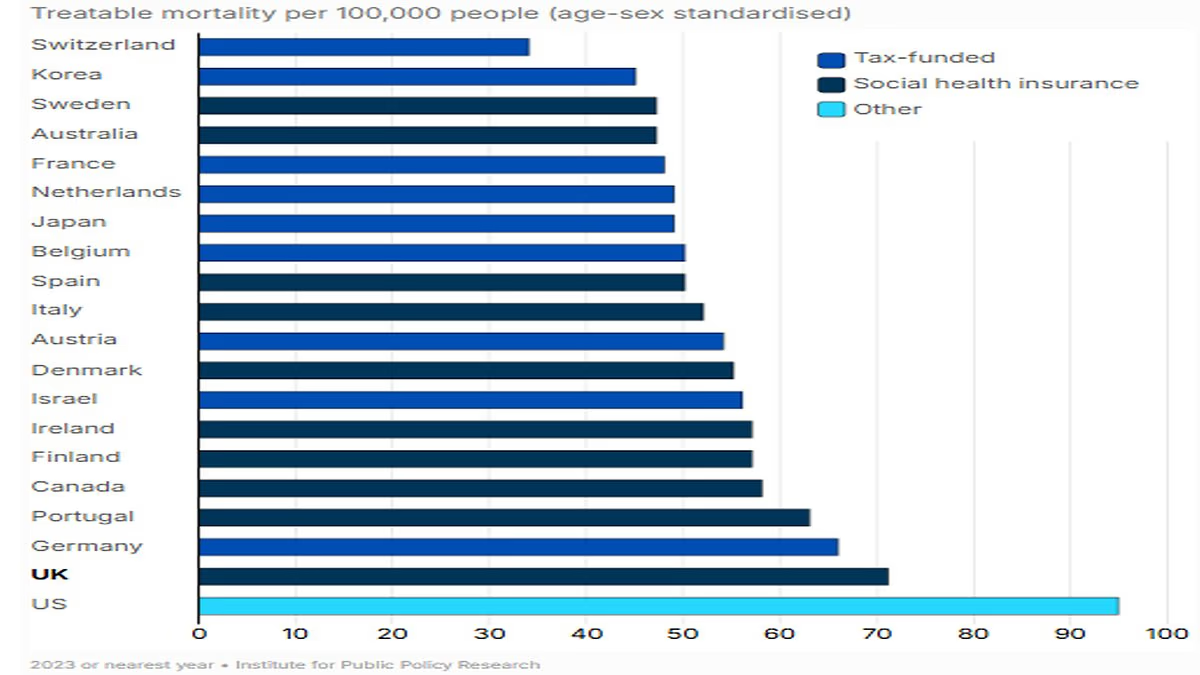
These findings are expected to intensify scrutiny of NHS survival outcomes, waiting times, and overall performance, as patients continue to experience prolonged delays in diagnosis and treatment across the UK.
Despite a substantial increase in health spending, which has risen by more than £60 billion in a decade to reach £242 billion annually, the NHS continues to lag behind comparable countries across a range of health indicators.
Experts have attributed this disparity to 'poorly targeted' funding, suggesting that a greater proportion of funds has been allocated to staffing and pay, while hospitals grapple with critical shortages of essential equipment, scanners, and infrastructure.
Specifically, the UK possesses only 19 MRI, CT, and PET scanners per million people, a stark contrast to approximately 50 in similar tax-funded healthcare systems and up to 68 in others.
Furthermore, the nation has fewer hospital beds than many comparable countries, a factor contributing significantly to longer waiting times and delays in both diagnosis and treatment.
These pressures are clearly reflected in international outcome measures, such as survival within 30 days of a heart attack, where the UK consistently performs below average.
The Telegraph reported these findings, also highlighting that Britain is among the worst performers for unmet medical needs, with patients frequently reporting difficulties in accessing timely care.
Widespread long NHS waiting lists for specialist appointments and elective surgery persist, leaving many patients waiting months for crucial treatment.
The Institute for Public Policy Research (IPPR) contends that years of chronic underinvestment in NHS infrastructure – encompassing hospitals, scanners, and technology – are the primary drivers of these systemic pressures.
Capital investment in the NHS remains at roughly half the level observed in comparable countries. While debates surrounding NHS reform are prevalent, researchers have dismissed a shift to European-style insurance systems as a 'pointless distraction'.
They assert that the fundamental issue lies in how NHS funding is allocated and invested, rather than in the funding model itself.
Health Secretary Wes Streeting has emphasized the necessity for NHS budgets to be spent more effectively, acknowledging that ministers face difficult choices and must ensure spending is 'well spent'.
He remarked on the timely nature of the report, noting, 'It dispels the myth that insurance-based healthcare systems are more efficient. While this Government is cutting the back office to reinvest in the front line, those who would rather move to an insurance system would do precisely the opposite.'
Streeting reaffirmed the NHS model as the fairest way to provide care, preventing wealth from dictating health outcomes. He underscored that the founding promise of the NHS from 1948 – that healthcare should be universally available without financial worry – remains as relevant today.
The IPPR report also brought to light broader concerns regarding NHS capacity, infrastructure, and long-term strategic planning. Separately, recent NHS England figures last week indicated that some trusts recorded a higher-than-expected number of deaths compared with statistical expectations.

Blackpool Teaching Hospitals NHS Foundation Trust recorded deaths 31.9%above expected levels, Medway NHS Foundation Trust saw deaths 30% above expected levels, and University Hospitals of Morecambe Bay NHS Foundation Trust recorded deaths 28.8% above expected levels.
The NHS, however, stresses that these figures are not a direct measure of quality of care and should not be interpreted in isolation as definitive evidence of poor performance.
It is worth noting that all three trusts are also among lower-ranked NHS organizations in national performance tables, with inspectors having previously identified concerns requiring further review.
You may also like...
The World Has Been Looking at the Wrong Map, and Nobody Thought to Question It

For over 450 years, the Mercator map has shaped global perception, shrinking Africa to the size of Greenland in the glob...
Nigerian Weddings Are Beautiful, But Are We Paying Attention to the Waste?

From endless aso ebi to overflowing food trays and single-use decor, Nigerian weddings are unforgettable for many reason...
₦13.66 Billion Went Missing in 2024, Nigeria's Fastest-Growing Payment System Has Some Questions to Answer

Nigeria processed ₦1.07 quadrillion in electronic transactions in 2024, yet a ₦13.66 billion NIBSS glitch remains unreso...
Why You Look Different in Mirrors, Selfies and Real Life (Science Explained)

Why do you look different in mirrors, selfies, and real life? This science-backed breakdown explains facial asymmetry, c...
Mbappe's Reign Continues: Real Madrid Star Secures Back-to-Back POTS Award
Kylian Mbappe has secured Real Madrid's Mahou Five Star Player of the Season award for the second consecutive time, high...
Wemby on the Spot: NBA Slams Star with Warning for Media Breach

The NBA has issued a warning to Victor Wembanyama for violating media access rules after he did not speak to reporters f...
News Emmys Shaken by Student's CBS Criticism Amidst Top Network Wins

The 47th News & Documentary Emmy Awards celebrated excellence in journalism, with ABC News leading wins and student Sant...
ARIA Hall of Fame Forges 'Historic First' Broadcast Deal: A New Era for Music Recognition

The Australian Recording Industry Association (ARIA) celebrates its 40th anniversary Hall of Fame with a special broadca...
