Breakthrough: HPV Vaccine Offers Hope for Male Cancer Prevention

A significant new study has revealed that boys who receive the latest version of the Human Papillomavirus (HPV) vaccine could substantially reduce their risk of developing various cancers.
The research, published by JAMA Oncology, analyzed health records from over three million young men and found that those vaccinated against nine strains of the virus had a 46 percent lower risk of HPV-related cancers overall.
This protective effect was consistent across both younger teenagers and young adults, demonstrating a tangible reduction in risk from approximately 12.5 cases per 100,000 in unvaccinated males to 7.8 per 100,000 among those who had received the jab.
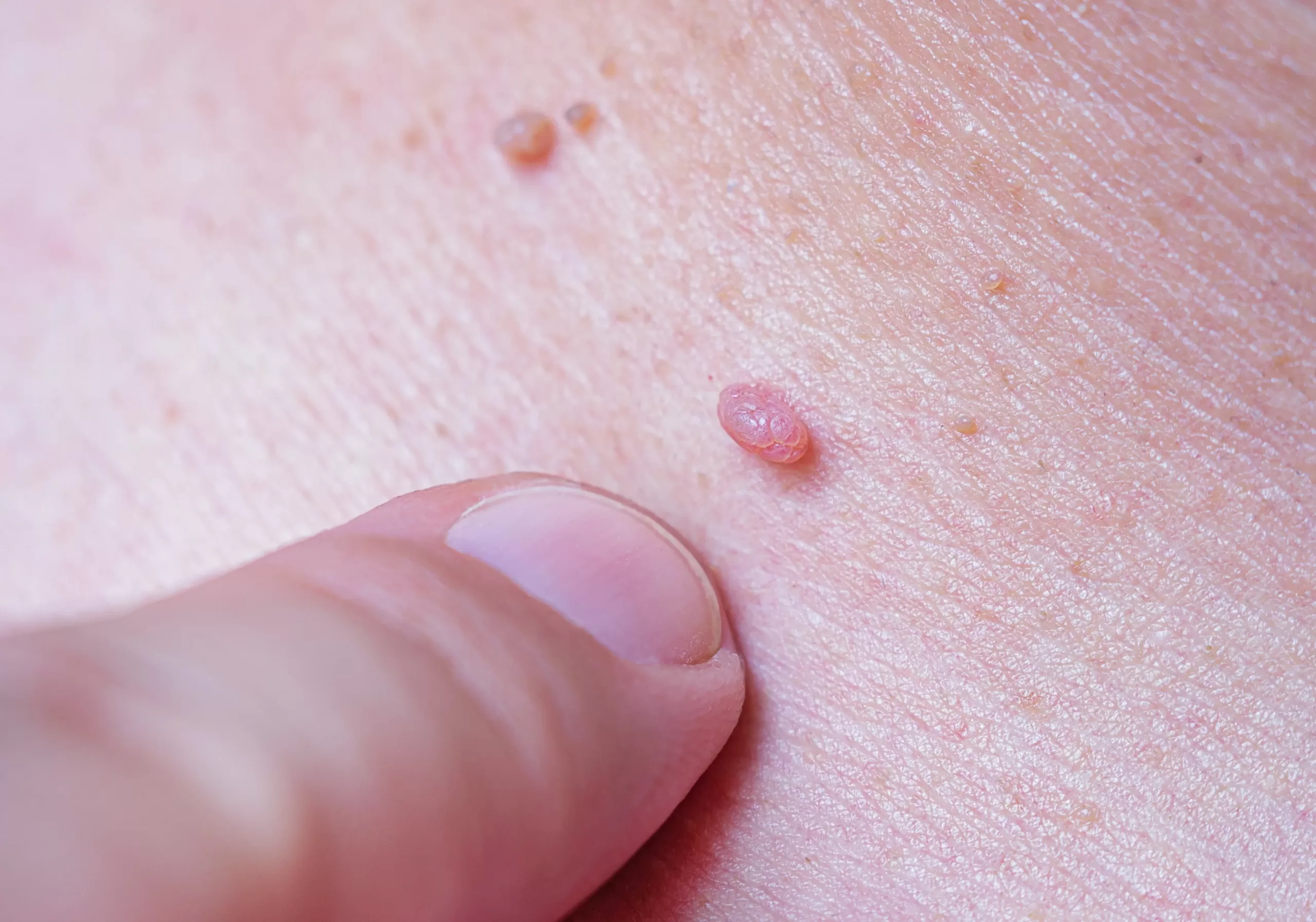
Human papillomavirus is an exceedingly common virus transmitted through skin-to-skin contact.
While often benign, certain high-risk strains of HPV are known to cause a range of serious diseases, including various cancers such as those affecting the head and neck, anus, and penis in men, as well as cervical cancer in women.
Historically, much of the evidence demonstrating the vaccine's efficacy in preventing cancer has primarily centered on women, particularly regarding cervical cancer.
Furthermore, previous research concerning men often focused on whether the vaccine reduced infection rates rather than its direct impact on cancer prevention.
This latest study marks a critical advancement, providing some of the clearest and most robust evidence to date that the HPV vaccine can directly protect men from cancer.
By directly comparing vaccinated and unvaccinated males, the findings offer a compelling case for expanding vaccination initiatives.
Scientists emphasize that extending HPV vaccination programs to include boys could play a pivotal role in reducing the overall transmission of the virus, directly safeguarding men's health, and accelerating the global decline in HPV-related cancer incidences.
Despite these profound findings, researchers did offer some important caveats. They noted that cancer cases in young men remain relatively rare, and it is also important to acknowledge that not all the cancers examined in the study are exclusively caused by HPV.
Additionally, the long-term impact of the vaccine will require follow-up over several decades to be fully understood. Nevertheless, the study's conclusive message is that the HPV vaccine is not solely for girls and holds significant potential in preventing cancer in men.
In the United Kingdom, the HPV vaccination program has already expanded to include all boys in Year 8 (typically aged 12 to 13) since September 2019, ensuring broader protection against HPV-related cancers.
This program, primarily delivered through school-based initiatives, targets high-risk HPV strains known to cause cervical, genital, and head and neck cancers.
Furthermore, men who have sex with men (MSM) aged up to 45 are eligible to request the vaccine for freethrough sexual health and HIV clinics in the UK, recognizing this group's potentially higher risk of anal cancer, which vaccination can help mitigate.
The study also highlighted that oral sex is considered a leading risk factor for HPV-related oropharyngeal cancer, a type of throat cancer, largely due to the transmission of high-risk strains such as HPV-16.
While a significant number of individuals contract oral HPV, most clear the infection naturally.
However, a small proportion can develop persistent infections that may progress to cancer over time, underscoring another critical pathway for HPV-related disease prevention through vaccination.
You may also like...
Super Eagles Gear Up for Unity Cup Opener Against Zimbabwe: New Captain, Fresh Vision!

The Super Eagles of Nigeria are set to defend their Unity Cup title against Zimbabwe in an experimental semi-final clash...
Arsenal Ends 22-Year Drought: Premier League Title Celebration Rocks Crystal Palace!

Arsenal has ended a 22-year wait, clinching the Premier League title with a 2-1 victory over Crystal Palace. This histor...
Mandalorian and Grogu's Box Office Struggle: A Debut Disaster

"The Mandalorian and Grogu" faces the daunting expectations of the Star Wars franchise, contrasting its $165 million bud...
Legend Returns: Neil Young Kicks Off 2026 with Vancouver Benefit Extravaganza!

Neil Young made a surprise return to the stage in Vancouver for David Suzuki's 90th birthday benefit concert, performing...
Drake Dominates Down Under: Superstar Shatters ARIA Chart Records!

Drake has shattered records on Australia’s ARIA Albums Chart, becoming the first artist to debut three new albums simult...
Opportunity Africa Kicks Off Bold Campaign to Spotlight Africans on Africa Day

Launched on Africa Day, the #NotWaiting campaign, spearheaded by Opportunity Africa, Africa No Filter, and Brand Africa,...
Nigerian Labour System Under Scrutiny: How It Keeps Fathers From Their Children

Nigeria's current labor laws, which largely omit paternity leave, compel fathers to return to work immediately after chi...
Fintech Powerhouses Velmie and Flot Unleash Digital Bank Across Africa

Velmie has partnered with Flot to develop a next-generation neobank for consumers and businesses across Africa, addressi...


