Shocking Misdiagnosis: Woman's 'Thrush' Revealed as Cancer, Crucial Symptoms for Every Woman

A 31-year-old woman from Bristol, Laura Liddle, has courageously shared her challenging journey with vulval cancer, which saw her initial symptoms repeatedly misdiagnosed as thrush by her general practitioner.
Ms. Liddle first noticed an unusual, non-painful swelling in her left labia in March 2022, shortly after recovering from surgery for an abscess in her groin. Initially, she dismissed the anomaly, attributing it to her anatomy.
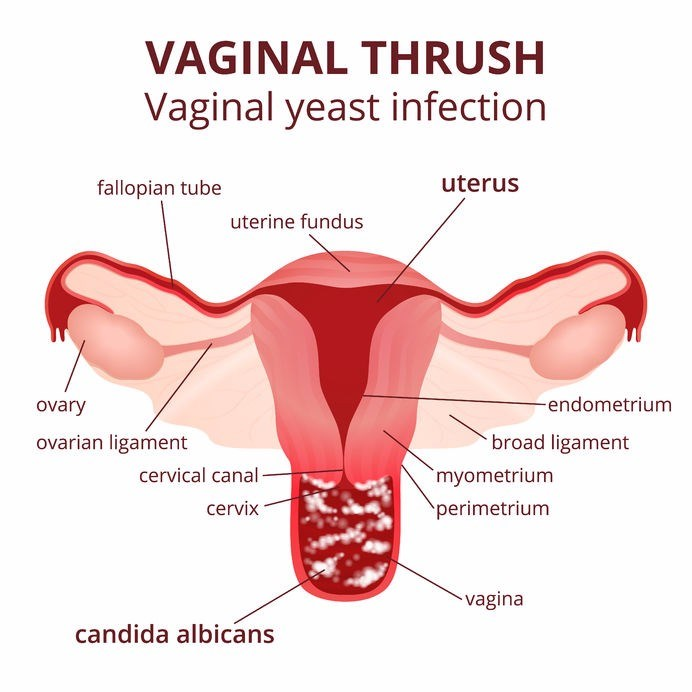
However, by January 2025, her condition had deteriorated significantly, leading to extreme genital pain that hindered her ability to walk, sleep, or even wear underwear. She vividly described the sensation as being 'stung with stinging nettles' between her legs.
Over the subsequent three months, Ms. Liddle made numerous, urgent visits to her GP. Despite her persistent discomfort, doctors conducted tests for thrush and STIs, all of which returned negative.
Having a history of thrush, she found that her doctors consistently attributed her escalating symptoms to this common condition, even after local anaesthetic gels proved ineffective.
It was not until April 2025, following a referral to a hospital gynaecology department, that a biopsy finally revealed the true nature of her ailment: stage three vulval intraepithelial neoplasia (VIN).
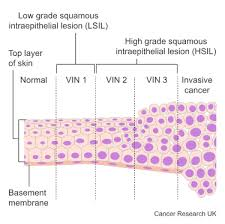
VIN is characterized by the presence of abnormal cells in the top layer of the skin of the vulva. While this condition can evolve into vulval cancer over many years, not every individual diagnosed with VIN will ultimately develop the disease.
Vulvar cancer itself is relatively uncommon, with only about 1,400 cases diagnosed annually in the UK. A significant majority, approximately 80%, occur in women over 60, whereas VIN is more frequently observed in women aged 30 to 50.
Crucial protective measures against vulvar cancer include the HPV vaccine, as many forms of the disease are triggered by the Human Papillomavirus, which is also linked to cervical, anal, and penile cancers.
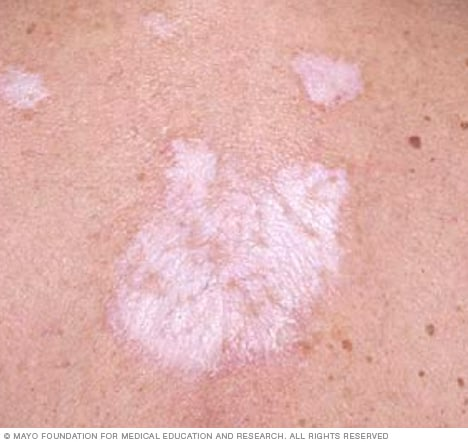
Another condition associated with vulvar cancer is lichen sclerosus, an inflammatory disorder that causes severe itching, discomfort, and the formation of white patches on the vulva. This chronic inflammation can also lead to the narrowing of the vaginal entrance due to scar tissue, with one in 20 cases potentially progressing to vulval cancer.
In July 2025, Ms. Liddle, who works in hospitality, underwent surgery to remove a portion of her labia. It was during this period that she received the devastating news that her VIN had, in fact, developed into vulval cancer.
Further surgical intervention followed in December 2025 to remove lymph nodes from her groin. Encouragingly, she was declared cancer-free on Christmas Eve of that year.
Despite this positive outcome, doctors cautioned Ms. Liddle that her sex life would likely be impacted, potentially becoming more painful and making it harder to achieve climax due to nerve sensation loss. She also continues to experience pain and burning during urination.
Reflecting on her ordeal, Ms. Liddle expressed that her primary concern upon receiving the cancer diagnosis was for her family. She noted the rarity of vulval cancer in women of her age, typically affecting those over 70, and believes her case may be linked to her immune system and HPV.
Adapting to her new normal at home, she grapples with physical challenges and emotional distress, stating, "I'm only 31, I shouldn't be having this happen to me. I like to work, I like to be busy and the fact I can't do anything is driving me insane."
Now a fervent advocate, Ms. Liddle is dedicated to encouraging women to overcome the societal taboo surrounding the examination of their own bodies.
She passionately urges them to regularly inspect their vaginas, familiarize themselves with what feels 'normal,' and promptly seek medical advice for any unusual changes, underscoring that such vigilance could be life-saving.
Furthermore, she strongly believes thatvulval cancer screeningshould be integrated into routine smear tests, suggesting that a visual check and, if necessary, a biopsy, though uncomfortable, represent "two minutes of pain for something that's going to save your life."
You may also like...
Should You Move Out at 25 or Stay Home and Build Wealth? The Question No One Really Prepares You For

Moving out at 25 is often treated as a milestone, but for many young earners it reshapes how fast they can build wealth....
Ethiopia Just Listed Ethio Telecom On ESX. The IPO Missed Its Target By 90%, And Nobody Is Leading With That

Ethio Telecom is listed on the Ethiopian Securities Exchange, but the IPO raised only 10% of its target, and that gap is...
DeepSeek V4-Pro Is Cheaper Than GPT-5.5 and Claude Opus 4.7 — So Why Is No One Using It?

DeepSeek V4-Pro is cheaper than GPT-5.5 and Claude Opus 4.7 and matches them in key benchmarks, but concerns over trust,...
Ebola Is Not the Only Virus Spreading in Congo

Ebola outbreaks in Congo are being worsened not just by the virus but by misinformation, mistrust, and attacks on health...
10 Everyday Rights You Should Know as a Nigerian, But Nobody Talks About

Many things Nigerians accept as “normal” are actually illegal. From unwanted landlord behaviors to fake “No Refund” sign...
Rangers Crowned NPFL Champions, Receive National Acclaim

Rangers International FC has made history by winning their ninth Nigeria Premier Football League (NPFL) title, earning c...
Super Eagles Gear Up for Epic Clash in Unity Cup
Super Eagles coach Eric Chelle has challenged Nigeria Premier Football League players to prove their worth amidst a squa...
Big Bang Theory Sequel Shocks Fans with 'Weirdest Reinvention' Yet!

The Big Bang Theory is set to launch a daring new spin-off, "Stuart Fails to Save the Universe," premiering on July 23, ...