What If Your Body Could Heal Arthritis Instead of Just Managing It?
Ask anyone who has watched a parent lower themselves slowly into a chair, wincing, bracing against the armrest, pretending they are fine, and they will tell you arthritis is not just a medical condition. It is a robbery.
It takes mornings, mobility, and dignity and it leaves behind pain that no amount of paracetamol fully reaches.
Osteoarthritis is the most common form of the disease, and it works like this: the cartilage cushioning your joints wears down over time, bone begins to grind against bone, and the inflammation that follows becomes your new permanent neighbour.
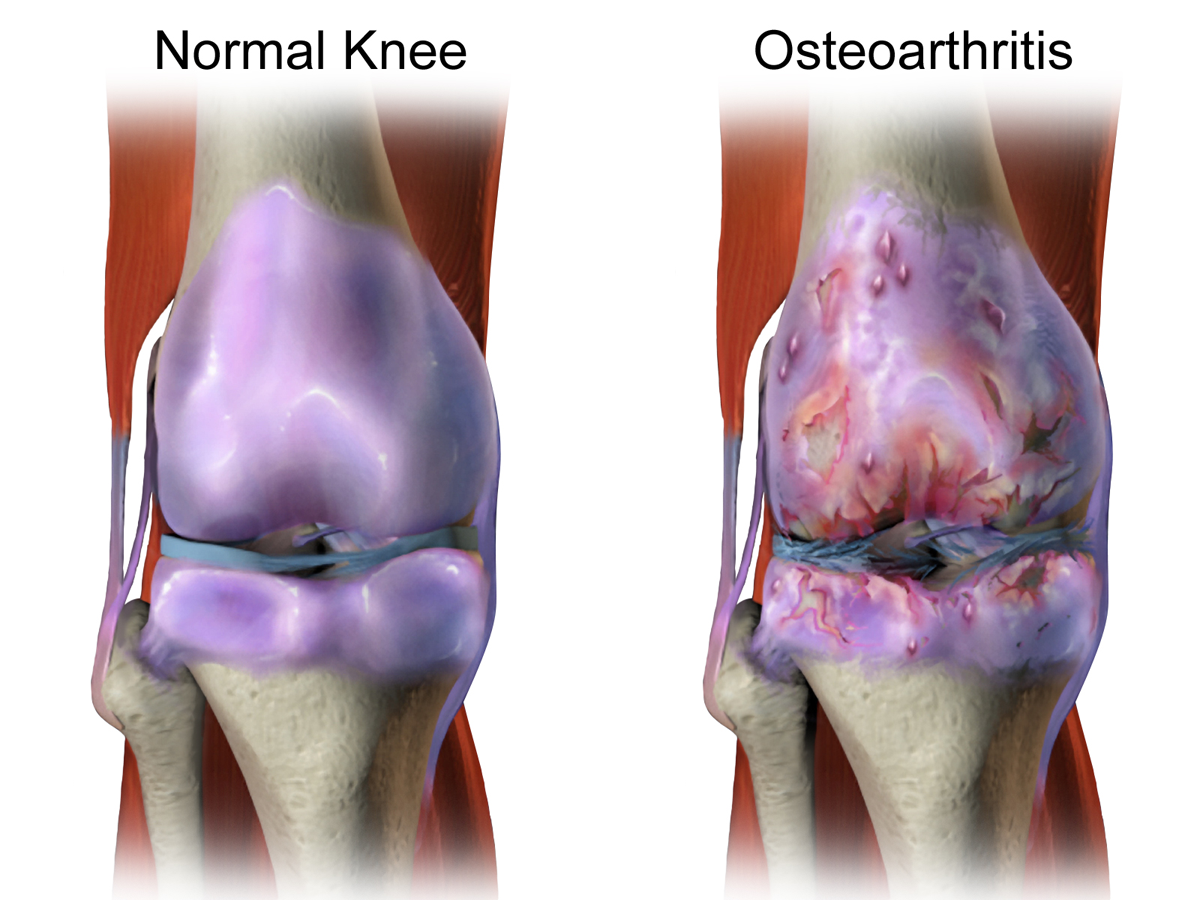
The world has largely accepted this as an inevitable feature of aging, as something to manage, not reverse.
Painkillers, injections and eventually, surgery have been the script that has barely changed in decades.
However, there is good news. That script might finally be getting rewritten.
What the Scientists Are Actually Doing
Researchers at Duke University, working alongside teams at UCLA, Boston Children's Hospital, and Harvard, have just hit a major milestone in developing something that sounds almost too good.
They discovered a therapy that does not just dull arthritis pain, but actually triggers the body to repair its own damaged joints.
The project, funded under the US government's Advanced Research Projects Agency for Health (ARPA-H), received an initial $13 million in 2024, and the team has now cleared its first phase of preclinical targets, putting them in line to receive up to $12.5 million more to push toward human trials.
What they are working on is three experimental drug combinations designed to activate the body's own regenerative processes, specifically in cartilage and the bone underneath it, which is where osteoarthritis causes the most destruction.
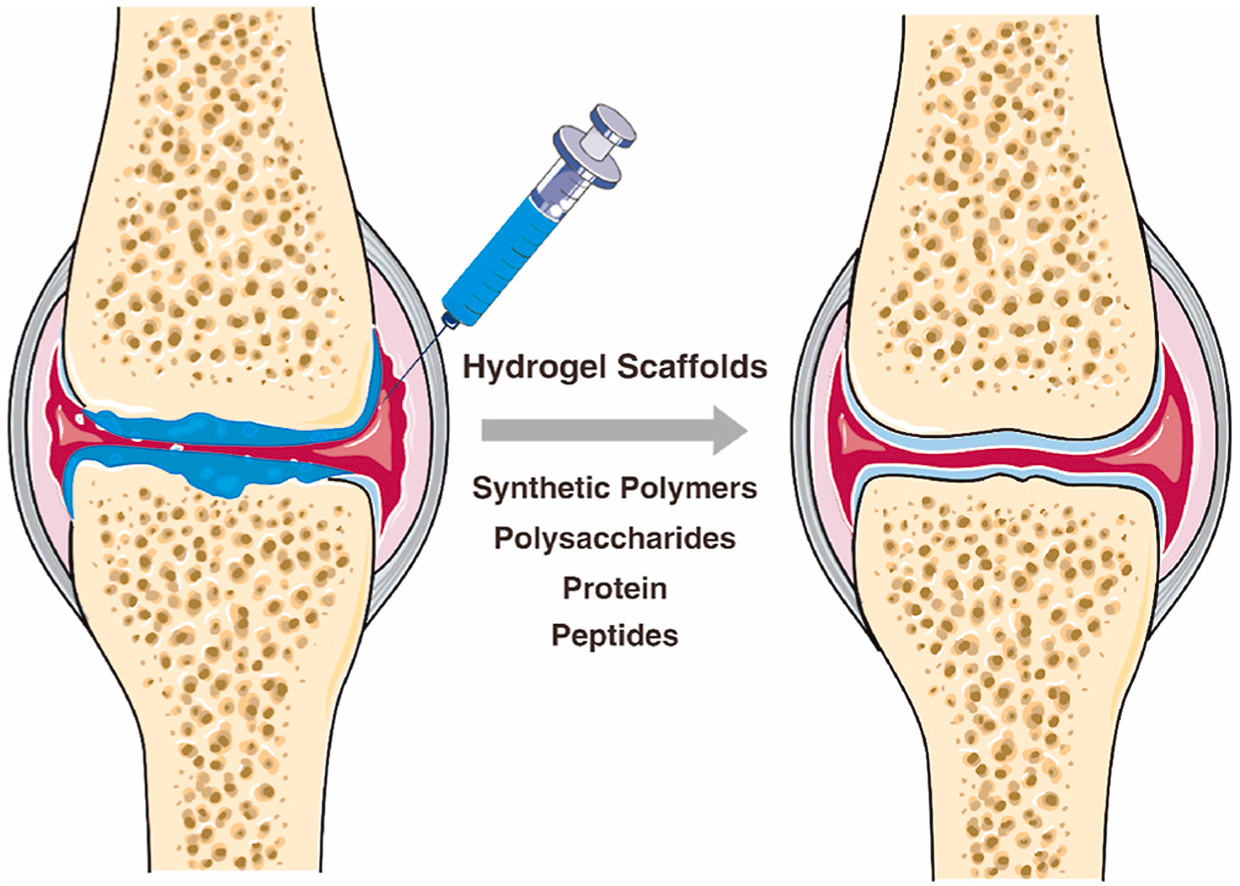
In animal models, the treatments restored joint tissue to near-normal levels and significantly reduced pain markers over extended periods. The team now moves into safety testing and dosing studies, with first-in-human clinical trials expected within the next 18 to 24 months.
The project lead, Dr. Benjamin Alman, said that the goal is to treat the root cause, not just the symptoms.

That one sentence carries enormous weight if you understand how far removed it is from everything that currently exists.
What About Africa?
Across Africa broadly, osteoarthritis is not just an older person's problem quietly happening in the background. It is a public health issue that is drastically underdiscussed.
Studies from Nigerian primary health care clinics have found the overall prevalence of physician-diagnosed symptomatic knee osteoarthritis at around 11.5%, with women affected at more than double the rate of men.
These numbers are from people walking into general clinics, often for something else entirely, who happen to have joint degeneration that nobody properly addresses.
Africa accounts for over 37% of the global osteoarthritis burden, yet the continent remains chronically underrepresented in research, underfunded in rheumatology care, and almost entirely absent from the conversations happening in well-resourced medical institutions abroad.
The Real Cost of Being Ignored
In Nigeria specifically, most people with osteoarthritis never receive a formal diagnosis, and joint pain is often invalidated as a serious chronic condition. Patients are frequently sent home with anti-inflammatory drugs and no real framework for understanding what is happening to their bodies.
There is no universally agreed clinical guideline for osteoarthritis care in Nigeria. The lived experience of people navigating this condition in low-resource settings includes limited access to physiotherapy, overreliance on medication as the primary care strategy and inconsistent advice that leaves patients confused and searching for answers.
It gets heavier. Research in Nigeria found that 42% of patients with symptomatic knee osteoarthritisalso showed evidence of depression, a finding that makes complete sense once you understand what unmanaged chronic pain does to a person's mental and emotional life over months and years.
Why This Breakthrough Matters
The Duke research matters globally, but it matters differently on this continent.
In contexts where joint replacement surgery is largely inaccessible, where physiotherapy is a luxury, and where the average patient cannot afford sustained pharmaceutical treatment, a regenerative therapy that works at the cellular level and potentially requires only targeted doses rather than lifelong medication, could be transformational.
It closes a gap that has been widening for decades between what wealthier countries can offer their patients and what the rest of the world quietly does without.
There is still a long road. Animal models are not humans, and clinical trials are notoriously unpredictable.
The therapy could look different by the time it reaches commercialisation, and questions of affordability and access will need to be fought for.
However, the idea itself matters. The idea that the body might be coached into healing rather than just sedated into tolerating pain is a different kind of medicine.
For the millions of Africans living in that slow, grinding daily reality, it is also a different kind of hope.
You may also like...
Usyk Dominates Verhoeven in Thrilling Knockout, Rematch Talk Ignites Boxing World

Oleksandr Usyk defeated kickboxing star Rico Verhoeven in a controversial eleventh-round stoppage during their heavyweig...
Netflix Shock: Blockbuster That Raked In 14x Budget in 8 Days Now Exits Platform

Erotic thrillers, led by 'The Housemaid' and 'Fifty Shades of Grey,' are experiencing a commercial resurgence, defying c...
Paramount+ Sci-Fi Fails: 136M Hour Video Game Adaptation Can't Fix Strategy

The live-action Halo TV series, despite high anticipation, ultimately disappointed fans and was canceled after two seaso...
Revolutionary Vision: Boots Riley's 'I Love Boosters' Unpacked

"I Love Boosters," Boots Riley's politically charged comedy-thriller, delves into a hyper-capitalist future through the ...
Amazon's Mysterious 'Bee' Wearable: Intrigue and Creepiness Unveiled

Bee, Amazon's AI wrist gadget, offers promising capabilities as a personal assistant for recording and summarizing conve...
Tinubu's Unstoppable Rise: APC Presidential Primary Dominates Headlines

President Bola Tinubu secured an overwhelming victory in the All Progressives Congress (APC) presidential primaries acro...
High Stakes: Iran-US Peace Deal Hangs in Balance Awaiting Crucial Approval

A proposed peace deal between the US and Iran is reportedly largely negotiated, offering sanctions relief and asset unfr...
Europe Outraged: Russia Unleashes Hypersonic 'Oreshnik' Missile in 'Deranged' Kyiv Attack

Russia launched a massive missile and drone attack on Kyiv, deploying its powerful hypersonic Oreshnik ballistic missile...






